
Hannah says her partner, Will, was an amazing support person during her second surgery for endometriosis. Photo: Supplied.
As a journalist, I’m always asking others to share personal stories so it seemed reticent not to share mine this March, which is Endometriosis Awareness Month.
I was 21 when I was diagnosed with the disease that’s since inhabited my uterus, ovaries, bladder and bowel.
It seems surprising now that I had never heard of endometriosis at the time, given it affects one in 10 women.
The most common symptom is debilitating period pain, and while my period had felt like a week-long war inside my uterus from the age of 15, I thought that was normal.
Every female complains of period pain, right?
However, what wasn’t normal was the vomiting I experienced or classes I missed because of the pain.
Yet it was bloating that stopped me in my twentysomething tracks. This wasn’t the kind of bloating you experience after indulging in a family pack of Tim Tams, but the kind that convinced me I was six months’ pregnant.
So I arranged to see my GP, who sent me off for ultrasounds. It was all very kosher and I was convinced there would soon be a simple solution – a change in diet, more exercise or less stress, perhaps.
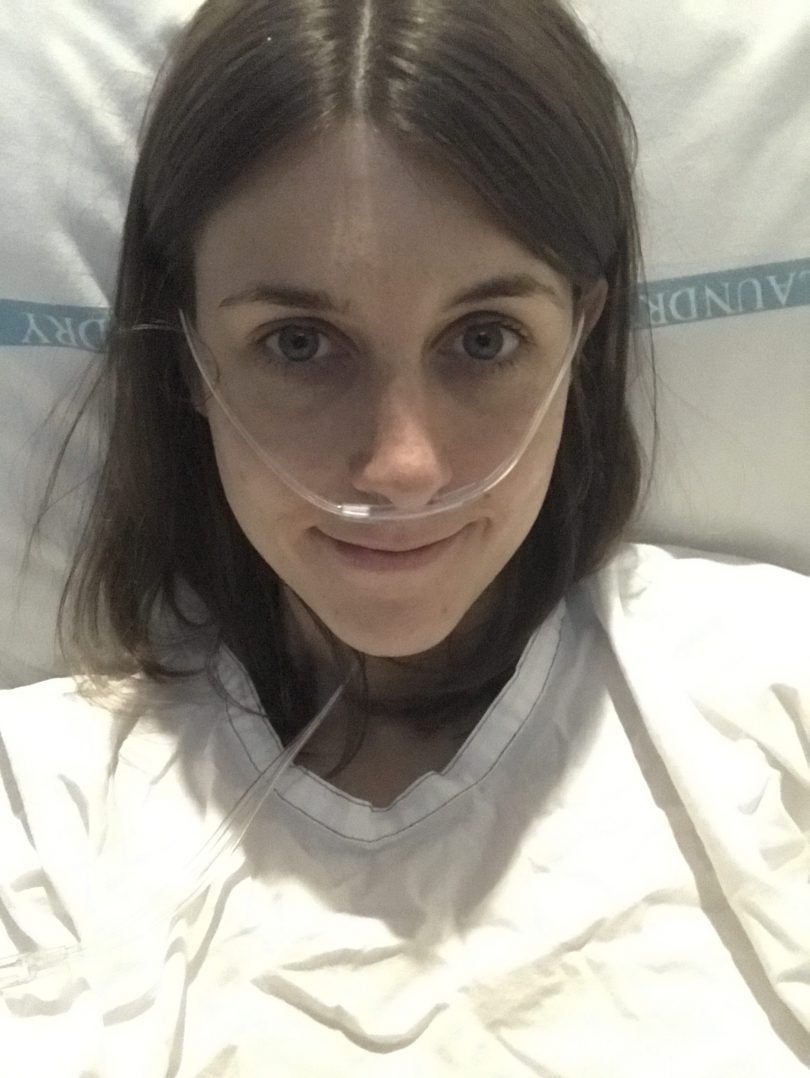
Hannah after post-laparoscopic surgery to remove endometriosis in February 2020. Photo: Supplied.
I remember opening the ultrasound results on a busy Sydney street (I never have had much patience). The words stood out at me: “Large, chocolate cysts, suggestive of endometriosis.”
Now I really wished I’d finished off that pack of double-coated Tim Tams.
Dr Google was my new best and worst friend between that day and my next GP appointment. I was able to get a handle on this unexpected news, however stories of horror surgeries and infertility were rife.
I was living my best years, for goodness sake, starting a career in the big smoke and partying away precious weekends. Yes, I wanted to have children someday, but that day seemed very far away.
It seemed insane that I’d soon be sat in a specialist’s office discussing how to freeze my eggs, especially when it cost $10,000 and I was lucky to have $100 in my account at the end of a fortnight’s pay.
At my next GP appointment, I explained to the locum doctor why I’d been sent for ultrasounds and that I had the results. He laughed, as if to suggest my GP had already gone to too much trouble for what he suspected was constipation.
Vulnerable and broken-hearted, I held back tears and held onto the fact I’d have some vengeance when he discovered what I already knew to be true.
This isn’t just a story about poor bedside manner, although I hope that doctor learnt a lesson. This is a story indicative of why thousands of women go undiagnosed for seven to 12 years after reporting symptoms to their GP – GPs who don’t know enough about endometriosis so can’t find a cause and say it’s all in your mind.
Let me tell you this: endometriosis isn’t all in your mind. You know your body better than anyone else. So find a doctor who hears you.
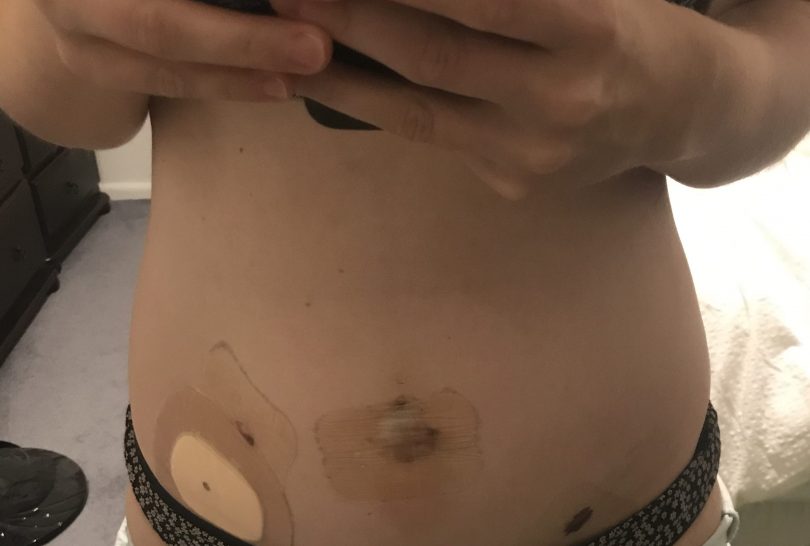
Hannah’s wounds from laparoscopic surgery. Photo: Supplied.
There are many myths surrounding endometriosis, including how falling pregnant is a cure-all. At least that’s what my first specialist recommended. Not only was I 21, but I was also very much single.
So then came specialist number two, who truly missed his calling as a lecturer. He proceeded to draw a horizontal line on a whiteboard, representing my fertility until it hit the big 3-0 drawn in black marker. That’s where the line came crashing down. Thanks, doc.
I knew by then that surgery was inevitable – the only way to properly diagnose endometriosis and end the pain.
My final specialist was a calm, optimistic chap. I appreciated his reassurance that I could still have children, as many people with endometriosis do. He recommended more ultrasounds before surgery to give him a better picture of the condition before opening me up.
Unfortunately, it was as the first ultrasound suggested so he booked me in for laparoscopic surgery to remove the endo through small incisions in my abdomen.
I’m now 30 and have had two surgeries in an attempt to remove the endometriosis. While the surgery is successful, the endo inevitably grows back every five years.
Unfortunately, there is no cure. I’ve found the Mirena hormonal intrauterine device, and removing dairy and gluten from my diet, have helped with the pain.
As for the future, I’m hopeful things will improve, but that is dependent on more education and funding.
To find out more about endometriosis, click here.
Among the books I’ve read on endometriosis are Please Read This Leaflet Carefully, The Doctor Will See You Now and How to Endo. I also follow @endometriosisaustralia, @endogirlgang and @me_myself_and_endometriosis on Instagram.








